After dropping her kids off at school each morning, Megan Colosino, PharmD, a clinical pharmacist in Ochsner Health’s Digital Medicine program, sits down at her home computer to start her day overseeing a large panel of patients with hypertension, diabetes and high cholesterol.
This year, the New Orleans–based health system celebrated the 10th anniversary of the program, which employs clinical pharmacists and physician assistants in a central role managing medications for patients with chronic conditions, plus offering weight management.
The nearly 30,000 patients nationwide who participate in Digital Medicine—available via their employers or insurance—are given Bluetooth-connected devices, including blood pressure cuffs and/or glucometers. Patients download the in-house Digital Medicine app and are encouraged to submit readings every day, or as often as possible, which get embedded in the electronic health record (EHR).
If values are out of range or trending in that direction, the system triggers an alert to one of the clinicians such as Dr. Colosino, who calls the patient to intervene or adjust their medication, documenting any updates in the EHR to inform patients’ primary care physicians.
The program’s 24 clinical pharmacists, all of whom have the equivalent of at least a PGY-1 residency, spend their days “100% focused on patient care,” said Valentina Williams, PharmD, the director of care delivery at Ochsner Health.
Each pharmacist has a dedicated panel of patients they monitor and a priority task list they follow, based on best-practice pathways and algorithms. Their overall goal is to focus on disease state control, patient engagement or other clinical targets. The pharmacists check patients’ blood pressure, glucose and other readings; talk to patients on the phone; and adjust medications as needed, working through a collaborative drug therapy management agreement with physicians.
“Our team works one-on-one with patients to achieve disease state goals,” Dr. Williams said. “Clinical pharmacists are key to the work we do, working collaboratively and as part of a multidisciplinary team with the patient’s primary care provider, physician assistants, health coaches, dietitians and more.”
Each morning, Dr. Colosino checks her messages to review new lab values and determines whether there are any questions from her patients, or from clinical providers about her patients, to answer. Then, she starts her outreach, making some 35 to 45 phone calls per day to patients who might require some type of management due to a high or low blood pressure alert, or to check how a patient is doing with a new prescription, or to touch base with a patient whose uncontrolled values might need a medication adjustment.
“It really is amazing what we’re doing from a pharmacist’s perspective,” she said. “We are able to use patient-entered data values to make optimal medication changes and follow up with the patients a couple of weeks after we make those adjustments.”
Program Slashes Hypertension Rates
The program started in 2015 as an internal quality improvement project to boost hypertension control rates among Ochsner Health patients, which then was about 60%, said Kenny Cole, MD, MS, the system vice president of clinical improvement at the health system and medical director of Ochsner Digital Medicine, during a presentation at HIMSS25, a global conference of the Healthcare Information and Management Systems Society, in Las Vegas.
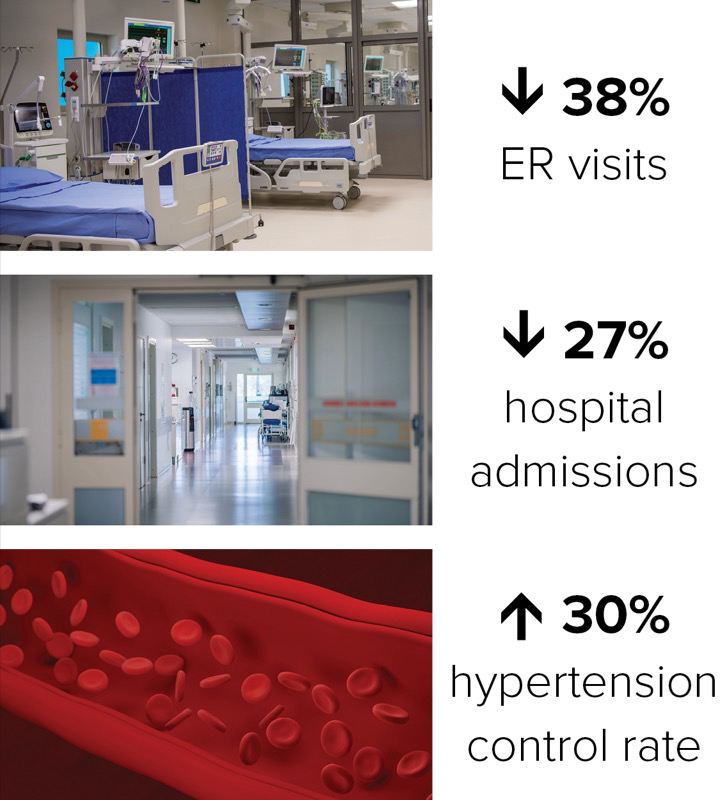
Although some were skeptical a hypertension control program could work in a state with high rates of obesity and salt intake, Dr. Cole said, a pilot study they had conducted found that if health-system physicians adhered to evidence-based protocols and pathways, 80% of patients could achieve hypertension control within six months. The program has since grown to encompass its health-system employees and is used by about 30 external clients—such as payors, employers and other health systems—for patients in 38 states, and is licensed in all 50 states. They now average more than 90% control rates for hypertension—a 30% improvement over baseline—and a similar outcome for diabetes.
Moreover, there has been a 38% reduction in ER visits and 27% decrease in hospital admissions among enrolled members, Dr. Cole said. Plus, less than 2% of patients leave.
The program also was designed to take some of the burden of managing these conditions off primary care physicians, said Dr. Williams, who was one of the first clinical pharmacists to participate. “Chronic care management is going to look a little bit different. It’s going to have to—there are not enough providers, there’s not enough time,” she said.
Many patients have achieved notable success, said Karly Bergquist, PharmD, a clinical pharmacist in the program. A patient she first encountered five years ago when she was training weighed more than 300 pounds and had a hemoglobin A1c level above 8%.
“Within three months of actively working with the clinician and the health coach, we were able to get her A1c to less than the prediabetes range,” Dr. Bergquist said. The patient continued to work on her health, losing more than 180 pounds and undergoing surgery to remove excess skin. “Now we’re focusing more on her hypertension management.” By reviewing the patient’s data, Dr. Bergquist was able to help identify a secondary cause of hypertension that may otherwise have gone unnoticed—primary hyperaldosteronism causing elevated blood pressure readings.
“What really gets me fired up about the role is a lot of our patients are in rural communities, and a lot of them are underserved,” she added. “The Digital Medicine program really allows us to increase access to care for these patients where they’re at, both physically as well as in their healthcare journey.”
A Boon for Physicians
Family medicine physician Victoria Smith, MD, an associate medical director of primary care and ambulatory quality leader at Ochsner Health in Kenner, La., said she appreciates the program as both a physician and participant. She estimates about 100 of her patients are enrolled, and she can see far more information on their disease through Digital Medicine than through typical, twice-yearly office visits.
In 2020, Dr. Smith herself was diagnosed with hypertension, and enrolled in the digital hypertension program. She requested a particular medication from her own physician, but once she started seeing the readings, she realized the medication she selected was not controlling her blood pressure.
“The pharmacist was able to connect with me and say, ‘Hey, why don’t we try a different medication?’” Dr. Smith said. “All of this happened on behalf of my primary care physician, and she didn’t have to either answer a message from me or put me on her schedule. Within about six weeks, working together with the clinical pharmacist, we found the right medicine.”
Every patient is assigned a clinical pharmacist for the duration of their time in the program and given their direct phone number, Dr. Bergquist said, “so you are able to really form those relationships.”
Dr. Colosino echoed those benefits. “If they’re having a side effect, instead of stopping that med on their own, they can call us,” she said. “We can discuss it. We can either help them through that side effect or change the medication just as quickly as we added it to be able to get the care that they need and still meet their goals for the program.”
Pharmacists in the program also work on best-practice guidelines specific to the management of patients in the digital medicine program “to ensure they have the best outcomes possible, not only for disease control but for preventing downstream complications,” Dr. Williams said.
Clinicians are now looking to expand into additional areas, including chronic kidney disease, atrial fibrillation and heart failure.
The sources reported no relevant financial disclosures beyond their stated employment.
This article is from the September 2025 print issue.