M ore than half of pharmacy directors polled in a new survey said that at least one of their residents failed to complete their PGY-1 programs, and about one-quarter noted that many of the residents who do graduate are electing not to pursue a PGY-2 position, according to data presented at the ASHP Pharmacy Futures 2025 meeting, in Charlotte, N.C.
A research effort done with ASHP has identified several causes of the PGY-1 dropouts, including an inability to pass the licensing exam, burnout and other mental health issues. The decline in PGY-2 residency matches is being fueled by concerns about salary and excessive workload, among other causes.
In 2025, 345 PGY-2 pharmacy residency positions went unmatched, per ASHP figures, compared with just 43 in 2020 (bit.ly/3TjvUsm).
There is widespread concern about these trends, noted Chelsea Keedy, PharmD, a clinical assistant professor of pharmacy at the University of Georgia (UGA) College of Pharmacy, in Athens, and a co-investigator on the research project. “These are questions that everyone is really interested in: residents, residency program directors, health systems and administrators. This affects everyone,” she said.
“I can attest that this is absolutely true,” said Meg Taylor, PharmD, the PGY-1 pharmacy practice residency director at Sentara Martha Jefferson Hospital, in Charlottesville, Va. “We’ve had a record number of residents not complete their [PGY-1] residencies in the last five to ten years, which wasn’t the case before. Previously, people committed to a residency and completed it.”
Beth Phillips, PharmD, an assistant department head for residency programs at the UGA College of Pharmacy, agreed. “We and a lot of other program directors have noticed there appears to be a decline in the number of residents finishing their first year and also in those going on to pursue a PGY-2 if they do finish that first year.”
To gain further insight into these trends, Drs. Phillips and Keedy, who are both part of UGA’s Ambulatory Care Collaborative research group, worked with ASHP and Qualtrics to develop the first large-scale survey to address concerns about declining PGY-1 completion rates and PGY-2 applicants (posters 38-S and 42-S).
The survey, sent from ASHP to all PGY-1 program directors of accredited residency programs, yielded 428 respondents spanning a variety of practice settings, with 196 (47%) from community hospitals, 120 (29%) from academic medical centers and the remainder from other institution types.
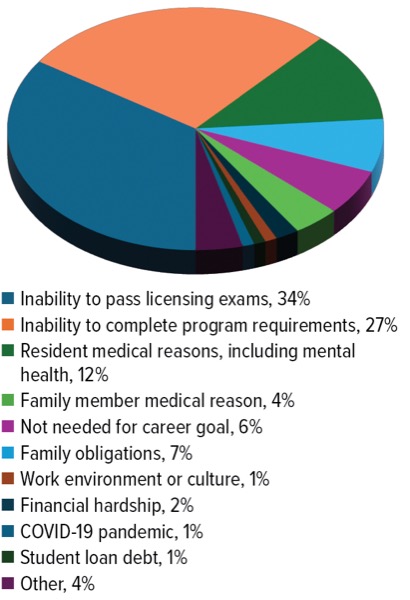
One section of the survey (poster 38-S) dug into program directors’ perceptions of reasons that their residents might not have completed their programs. More than half of the respondents (n=214; 51%) indicated having at least one PGY-1 resident who did not complete their residency in the last five years. The survey also gave program directors the opportunity to elaborate on their responses in free text sections. On the issue of PGY-1 non-completion, the comments coalesced around the larger theme of difficulty passing licensure exams and lack of preparedness for the requirements of residency programs, especially after the pandemic (Figure 1).
“I have seen an overall increase in the amount of educational remediations, as incoming residents do not seem as prepared for the workload of residency as they once did,” one respondent said. Another noted, “we have had two-thirds of our most recent residents require multiple exam attempts.”
Delaying NAPLEX a Concern
The general theme of difficulty passing examinations “has been a significant issue,” Karen Gunning, PharmD, a professor of pharmacotherapy and family and preventive medicine at the University of Utah, told Pharmacy Practice News. “The only pharmacy students who have a deadline to take the NAPLEX are those going into residency programs, and we’ve seen a lot of students delaying when they take it the first time,” said Dr. Gunning, who has been a member of the Utah Board of Pharmacy for the past six years. That delay is a concern because “[data suggest] this has a negative effect on passing,” she added. “Residents should take the exam as soon as possible, so that if you have trouble, you can take it again.”
Dr. Taylor agreed. “We are definitely seeing lower pass rates on the NAPLEX and other licensure exams,” she said. “In our organization, PGY-1s have 90 days from the first day they start work to get licensed, which is tough if you don’t already have an exam scheduled. I’ve also seen residents come in saying that they took the whole month of June off to relax, figuring they could study once residency started. But waiting to start preparing until you’re actually in your residency puts you way behind.”
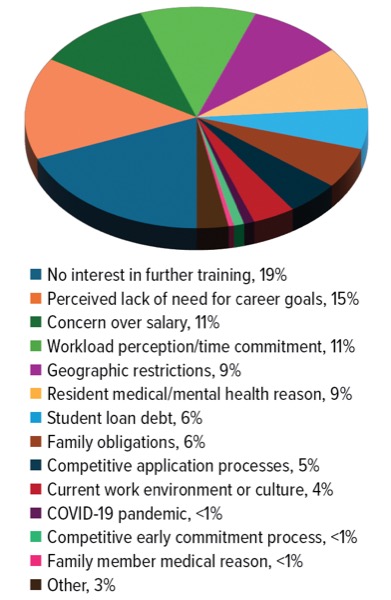
When program directors were asked about any decline in residents pursuing PGY-2 training (poster 42-S), 110 (26%) reported noting that fewer of their residents were seeking such training over the past five years (Figure 2). In this section of the survey, comments centered on the idea that trade-offs around completing a PGY-2 year outweighed the potential benefits, and the lack of need for specialization to enter the pharmacy workforce.
“Burnout is consistently a concern expressed by residents. PGY-1 is harder than they expected, and they are not enthusiastic about continuing to work that hard in a PGY-2,” one respondent said. Another noted that “ambulatory care, in particular, has been a struggle for our system as PGY-1 residents interested in that field commonly seek (and secure) jobs in it without PGY-2 training.”
Two Years Without a PGY-2 Ambulatory Care Resident
At the University at Buffalo in western New York, Nicole Albanese, PharmD, a clinical associate professor of pharmacy and PharmD program director has gone two years without a PGY-2 resident in her ambulatory care pharmacy residency. “Last year, I had two applicants, only one of whom was viable, and that resident went elsewhere,” she said. “This year, we had two applicants who were interested, but only one applied. He was amazing, but because he was amazing, he had the opportunity to go anywhere, and it wasn’t going to be Buffalo because he wasn’t from here.”
While Dr. Albanese said she firmly believes that ambulatory care is a pharmacy specialty that does require additional training to make it work, she acknowledged that that sentiment is not universally shared. “A hospital administrator will say, ‘They can learn it on the job—how to treat diabetes and hypertension in the clinic, how to make adherence calls and do all of these quality metric tasks.’ That would never happen with an oncology pharmacist or an ICU pharmacist.”
For Dr. Taylor, finances and burnout are indeed two key factors driving PGY-2 residency candidates elsewhere. “A lot of students are graduating with more debt these days, and [residencies are] a big financial burden to undertake if you’re not sure whether that extra year of training will [yield a higher salary]than just taking a job straight out of the first year of residency.”
ASHP’s Take
Asked to comment on the results, ASHP offered the perspectives of Sam V. Calabrese, BSPharm, MBA, FASHP, the group’s vice president for accreditation services. Mr. Calbrese first underscored the value of PGY-1 PGY-2 residencies. “Completing a PGY-1 residency gives learners broad-based skills in many different areas for generalist practice,” he said. “PGY-2 training provides residents with an opportunity to develop high-level skills in a specialty, so that they enter their preferred area of practice immediately with the necessary leadership and patient care skills.”
He added that in the short term, “ASHP will be reviewing messaging on PGY-2 training to highlight the value brought to a resident interested in a specialized practice. We will also look to gain insight from residents for a greater understanding of the issue.”
Mr. Calabrese cautioned, however, that “these are the initial results of the survey, so it’s too early to fully understand the implications. We are continuing to work on this topic; additional results from the survey are forthcoming. Once our analysis is complete, the data will be valuable for understanding resident and program needs so ASHP can better support programs and trainees.”
The sources reported no relevant financial disclosures.
This article is from the July 2025 print issue.