For critically ill patients, timely nutritional support can aid recovery and reduce mortality risk. But what about a patient in septic shock who is receiving vasopressor therapy, or one who requires prone positioning or extracorporeal membrane oxygenation (ECMO)—what should be the feeding strategy?
Using a case-based approach, three speakers discussed the feeding challenges for some of the most difficult-to-treat ICU patients during the ASPEN 2024 Nutrition Science & Practice Conference, in Tampa, Fla.
Angela L. Bingham, PharmD, BCPS, BCNSP, BCCCP, the acting chair and a clinical associate professor at St. Joseph’s University’s Philadelphia College of Pharmacy, focused on “this often highly controversial question of whether to feed or not to feed in the setting of enteral nutrition [EN] and vasopressors.”
This case involved “Haley”, 37, who was admitted to the medical ICU in septic shock. Her blood pressure was 70/65 mm Hg; mean arterial pressure (MAP) was 67 mm Hg; and body mass index was 15.5 kg/m2, placing her at significant risk for refeeding syndrome, Dr. Bingham noted. Based on these findings, she added, the patient required “conservative initiation of caloric provision and vigilant monitoring for electrolyte abnormalities.”
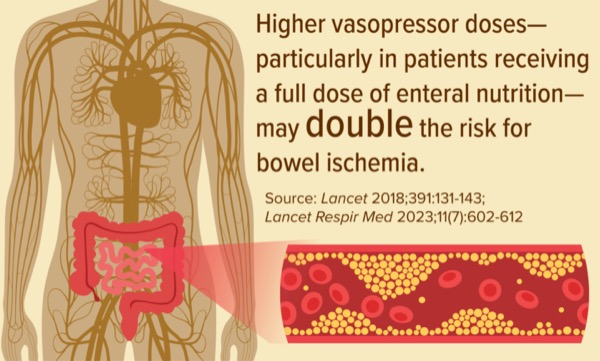
The patient, a composite drawn from critically ill patients to illustrate the session’s theme, was given vasopressor therapy consisting of norepinephrine 0.5 mcg/kg per minute and vasopressin 0.03 units per minute, both by continuous infusion. Dr. Bingham pointed out that use of norepinephrine, vasopressin and other vasopressors can “shunt blood to the heart and away from other organs like the gastrointestinal tract.” In about 1% of the cases, she noted, the reduced blood flow to the GI tract can result in necrosis (J Parenter Enteral Nutr 2022;46[7]:1470-1496). “That is why [this] clinical question is before us today.”
Dr. Bingham reviewed some of the “best available evidence” and consensus guidelines to help clinicians navigate “the delicate balance” between enteral feeding and hemodynamic management. Two clinical trials (NUTRIRERA-2 and NUTRIRERA-3) considered together, she said, “point out that higher vasopressor doses—particularly in patients receiving a full dose of EN—may increase the risk of bowel ischemia.” In NUTRIREA-2, she noted, EN compared with parenteral nutrition was associated with a higher cumulative incidence of bowel ischemia (2% vs. <1%; P=0.007), perhaps due to the high vasopressor dose (mean norepinephrine dose, 0.56 mcg/kg/min). In NUTRIREA-3, patients receiving early caloric and protein restriction compared with standard targets experienced less bowel ischemia (P=0.03) (Lancet 2018;391:131-143; Lancet Respir Med 2023;11[7]:602-612).
Next, Dr. Bingham turned to the 2016 guidelines from ASPEN and the Society for Critical Care Medicine, which addressed the safety and efficacy of EN in adult critically ill patients during periods of hemodynamic instability (J Parenter Enteral Nutr 2016;40[2]:159-211). She noted the guidelines’ position that the “cautious use of enteral nutrition” was deemed acceptable “in patients receiving chronic, stable, low doses of vasopressors.” However, she said, the guidelines called out specific cases when EN should be held, including patients with a MAP less than 50 mm Hg at vasopressor initiation or those receiving escalating vasopressor doses.
Additional caution should be taken, Dr. Bingham said, in patients with “signs of enteral nutrition intolerance, such as abdominal distension, increased nasogastric output, decreased passage of stool, hypoactive bowel sounds or increased metabolic acidosis.”
Dr. Bingham stressed the importance of MAP as a key indicator for feeding decisions, with a MAP of 60 mm Hg as the minimum point for initiating EN. She added, however, that vasopressor dose equivalent (VDE) also required attention. “So, when considering feeding in this particular patient population, we should initiate enteral nutrition within 48 hours of vasopressor initiation if our VDE score allows.” Also recommended, she added, is an EN formulation that provides 1 to 1.2 Kcal/mL, rather than a higher caloric density product (J Parenter Enteral Nutr 2022;46:1470-1496).
The route of administration for EN is also important, Dr. Bingham said, noting that gastric feeding is preferred to post-pyloric feeding in patients receiving vasopressors. “Unfortunately, a greater incidence of mesenteric ischemia has occurred in patients receiving feeding into the jejunum,” she said, especially in trauma, burn and surgery patients (J Parenter Enteral Nutr 2022;46:1470-1496).
Risks From Prone Positioning
Feeding patients who are in the prone position poses another ICU nutrition challenge. “You’ve all had this situation occur, especially if you’re in the ICU,” said Jan Powers, PhD, RN, CCRN, NE-BC, the director of nursing research and professional practice at Parkview Health, in Fort Wayne, Ind. “We resuscitate the patient and everything’s going great. Then they start to experience respiratory complications. Now we’re going to prone them, and the question is, what do we do with feeding?”
Prone feeding remains controversial, “but it shouldn’t be,” Dr. Powers stressed. “Although there are some people who are still concerned about safety and the risk of aspiration, there is research to support safety when feeding in the prone position.”
When can EN be started for patients who require prone positioning? Dr. Powers noted that the European Society for Clinical Nutrition and Metabolism 2019 guidelines suggest early EN initiation (Clin Nutr 2019;38[1]:48-79). “However, if you are feeding gastric in the prone position, you might want to consider measuring gastric residual volume [GRV]—that is, unless they’re tolerating gastric feeding,” she said. “Measuring GRV can show if the patient is tolerating gastric feeding.”
If the GRV is large, she explained, “you would want to add a prokinetic agent to stimulate gastric emptying or divert to post-pyloric placement.”
Another issue is whether the feeding tube should be placed before or after proning, Dr. Powers noted. One meta-analysis, she said, suggested that clinicians should ensure tube access before turning the patient (Nutr Clin Pract 2021;36[1]:105-109). “The best practice would be to place the feeding tube prior to prone positioning. If you are feeding gastric, it is much easier and quicker to place,” Dr. Powers said. “Prone positioning is an urgent procedure if a patient is decompensating, so it is not possible to take the time to place a feeding tube, especially post-pyloric.
“If the patient is going to be prone 16 to 20 hours, or sometimes longer,” she added, “and if there is no feeding tube, you are delaying nutrition by almost a day. One of the first studies on this topic found it was easier to place tubes in the prone position, and the success rate was higher than in the supine position” (Can J Anesth 2005;52:1106-1107).
During the COVID-19 pandemic, Dr. Powers and her team developed a novel technique for placing feeding tubes in prone-positioned patients. They used an electromagnetic placement device to guide small-bore feeding tubes within the pyloric region in 68 mechanically ventilated patients. “We were able to decrease the time from admission to enteral nutrition by over two days.” The team described the method in a 2023 study (Nutr Clin Pract 2023;38[3]:602-608).
Dr. Powers clarified that she was not advocating that everyone start placing tubes while patients are in the prone position. “You really need to have a very mature feeding tube team,” she said.
Dr. Bingham is a speaker for Abbott Nutrition Health Institute. Dr. Powers is a member of Medtrition’s clinical advisory board and a speaker for Stryker Medical and Avanos Medical. Ms. Modir reported no relevant financial disclosures.
This article is from the September 2024 print issue.