More malnutrition tests are needed in the outpatient oncology setting to improve patient outcomes, experts noted during a panel at the ASPEN 2025 Nutrition Science & Practice Conference, in Columbus, Ohio.
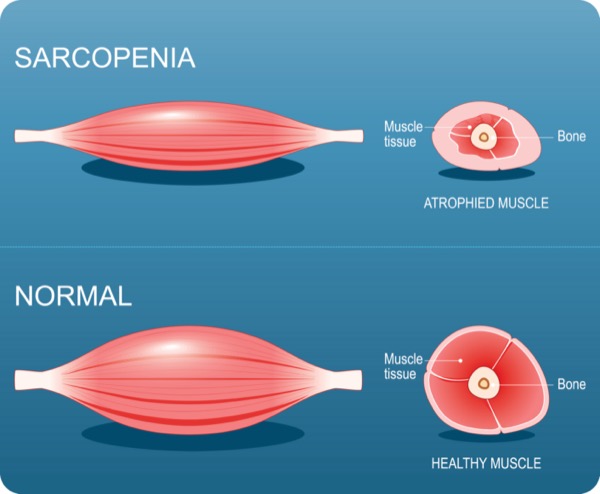
Malnutrition and sarcopenia are independent predictors of death in patients with cancer (J Cachexia Sarcopenia Muscle 2023;14[4]:1775-1788). Data from a 2024 study published in the Journal of Parenteral and Enteral Nutrition indicate that one-third of patients treated in ambulatory cancer centers (ACCs) present with a risk for malnutrition before treatment (2024;48[8]:874-894).
“We observed that having some risk of malnutrition based on a pretty simple [validated] patient-reported outcome measure was independently associated with survival when we controlled for cancer type, stage, timing of diagnosis, BMI [body mass index], weight and a number of other prognostic variables,” explained Kunal C. Kadakia, MD, the section chief of oncology nutrition and research in the Department of Supportive Oncology and Solid Tumor Oncology at Atrium Health Wake Forest Comprehensive Cancer Center, in Charlotte, N.C. “However, malnutrition in cancer patients treated in the ambulatory setting remains rarely identified.”
Despite the potential benefits of widespread malnutrition screening in ACCs, several implementation challenges exist. First, the obesity epidemic has made it difficult for clinicians to identify malnourished patients. “In fact, some of my patients [who present as obese] tell me, ‘Hey, I’m happy I’ve lost weight,’ and these patients are severely sarcopenic on their CT [scan] and are dying from their cancer,” Dr. Kadakia said. “It’s easy for any clinician—even someone like myself—who cares about this issue to overlook a malnourishment screening test in the midst of the obesity epidemic.”
Furthermore, the lack of mandates for malnutrition screening from organizations such as the National Comprehensive Cancer Network, coupled with a severe shortage of registered dietitian nutritionists (RDNs), means that convincing stakeholders of the feasibility of malnourishment screening in the outpatient setting is an uphill battle.
However, Colleen Spees, PhD, a professor in the Division of Medical Dietetics at The Ohio State University College of Medicine, in Columbus, advocated for consistent use of validated malnutrition tests across ACCs. “When we screen for malnutrition and intervene, we decrease hospitalization time and reduce time to treatment,” Dr. Spees said, adding that such efforts also potentially save money and clinicians’ time. As such, she recommended that all patients presenting to an ACC undergo malnutrition screening by a trained nutrition professional at intake and throughout treatment, using one of six validated tools:
- Malnutrition Screening Tool (MST)
- Malnutrition Universal Screening Tool
- Nutri-Score
- Nutrition Risk Screening-2002
- Patient-Generated Subjective Global Assessment Short Form
- Mini Nutritional Assessment
Dr. Spees said she also believes that patients who are identified as at risk for malnutrition should be given a follow-up plan that specifically addresses their nutritional deficits.
Keys to More Widespread Use
For widespread malnutrition screening in ACCs to become a reality, Dr. Kadakia noted, increasing visibility of RDNs and their economic and clinical value is essential. However, Dr. Kadakia, Dr. Spees and panel member Jeannine Mills, MS, RDN, CSO, LD, CNSC, a clinical dietitian in the Outpatient Oncology Department at Dartmouth Cancer Center (DCC), in Lebanon, N.H., also emphasized that malnutrition testing must be efficient, affordable and not a burden on clinicians if it is to be adopted. Ms. Mills described DCC’s model, which meets these requirements and might be implemented at other cancer centers.
At DCC, the MST is built into the electronic health record; RDNs are embedded in oncology teams, do not bill for clinical services and focus on raising awareness about the value of optimized nutrition management to their teams and patients.
Strength in Numbers
One of their most effective strategies is not relying on any single clinician to refer patients to RDNs for counseling. Ms. Mills and her fellow dietitians receive referrals from a wide range of clinicians. In fact, through efforts to raise the profile of RDNs on the cancer team, the referral of patients for nutritional counseling has become organic, reaching all the way to the pharmacy.
“We often get referrals through pharmacy because they’re doing chemo teach, or they’re doing a symptom check on the second cycle of chemo,” Ms. Mills said. “Oftentimes we’ll get a staff message from one of the pharmacists saying, ‘Hey, this patient is not doing so great. Can you help?’ These experiences show that when RDNs have visibility and a seat at the table, we can really help patients.”
Pharmacists as ‘Key Players’
Panel moderator Anne M. Tucker, PharmD, BCNSP, FASPEN, a clinical pharmacy specialist in critical care/nutrition support at The University of Texas MD Anderson Cancer Center, in Houston, echoed Ms. Mills’ sentiments, concluding that “pharmacists can be a key part in identifying patients who are suffering from malnutrition that are in between being seen by [a clinician] who is 100% dedicated for that screen.”
Drs. Kadakia and Spees and Ms. Mills reported no relevant financial disclosures. Dr. Tucker is a consultant to UpToDate Inc.
This article is from the May 2025 print issue.