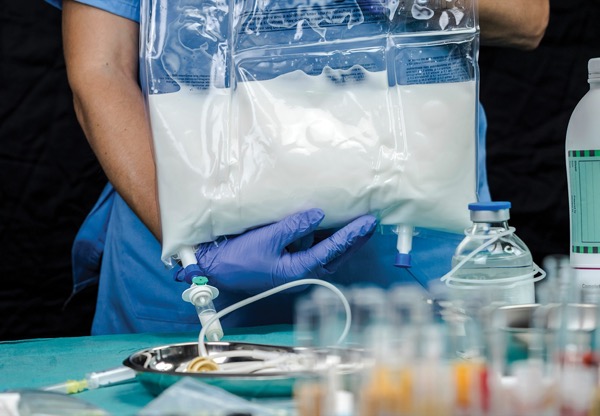
Pharmacists managing patients on parenteral nutrition (PN) are accustomed to dealing with shortages; these medications have been atop the FDA and ASHP drug shortage lists for years. But the problem intensified with the one-two punch of last September’s Hurricane Helene forcing the temporary shutdown of the Baxter plant in North Cove, N.C., that produces 60% of the country’s IV fluids, and the October announcement by CVS Health that its Coram infusion pharmacy subsidiary—one of the biggest home infusion pharmacies in the country—would be dropping its PN and IV antibiotics business.
These supply chain disrupters underscore the need for proactive PN shortage planning for 2025—particularly since PN shortages are a significant risk factor in an already high-risk drug therapy, said Sara Bliss, PharmD, BCPS, BCNSP, BCCCP, FASPEN, a clinical pharmacist specializing in trauma and nutrition support at the University of North Carolina at Chapel Hill. “Depending on the specific product, sometimes there might be alternatives like electrolytes, or maybe some alternative macronutrients,” Dr. Bliss noted during a session on PN safety at the ASHP Midyear 2024 Clinical Meeting & Exhibition, in New Orleans. But with the aftermath of Hurricane Helene, “we’ve even seen our macronutrients affected, like concentrated dextrose and sterile water for injection and then IV fluids,” she said. “When your primary, secondary and then third-line ingredient are all out of stock, that’s when things get very tricky, putting patients at risk for micronutrient deficiencies, dehydration, acute kidney injury and hospital readmission.”
PN is a high-risk medication, and patients who require it are at risk for medication-related errors and nutritional deficiencies that can have significant effects on health outcomes, she said. “The PN-use process has many opportunities for error related to the complexity of PN prescriptions. Additionally, patients may have preexisting nutritional deficiencies that have nonspecific symptoms and may go unnoticed or undiagnosed.”
Pharmacy Education Gap
In an interview with Pharmacy Practice News, Dr. Bliss noted that nutrition is minimally taught in undergraduate pharmacy degree programs. “I teach at Campbell University [College of Pharmacy & Health Sciences, in Buies Creek, N.C.], and their curriculum includes three hours of nutrition in total, which I honestly think is probably a lot compared with some other programs.” In fact, much of pharmacists’ training in PN has been pushed off to residency “because it is a more advanced area of practice and builds on foundational concepts,” she added. “But then not every residency program has these opportunities either.
“As a profession, I think we have left much of PN management to our dietitian colleagues, when really it should be a multidisciplinary partnership,” Dr. Bliss said. “As pharmacists, we obviously specialize in shortage management. If we don’t know the product well, how can we help to reliably manage PN shortages?”
Given the limited amount of training available in PN and the many ongoing shortages, pharmacy trainees may have only observed and experienced PN management in a time of shortage and not ever have been exposed to the more standard dosing of these products, she said. “Rationing PN components may result in ongoing knowledge deficits on standard macro- and micronutrient dosing, which puts patients at further risk for nutritional deficiencies.”
Dr. Bliss urged pharmacists to consider pursuing certification programs and credentials in nutrition support, such as the one offered by ASHP in partnership with the American Society for Parenteral and Enteral Nutrition (ASPEN) and the Nutrition Support Pharmacy Specialty Certification, which is overseen by the Board of Pharmacy Specialties (bit.ly/4gsJpjt).
“Taking those extra steps to get some of that additional training demonstrates that your institution recognizes that PN is a high-risk medication and needs someone with expertise on staff to guide these decisions,” she said.
Critical Care Settings
The ASHP Midyear session also focused on evolving PN practices in the critical care setting. ASPEN’s 2022 critical care nutrition guidelines (JPEN J Parenter Enteral Nutr 2022;46[1]:12-41) note that the evidence finds no significant difference in clinical outcomes between early exclusive PN and enteral nutrition (EN) during the first week of ICU admission, said Sarah Cogle, PharmD, BCCP, BCNSP, a clinical pharmacist specialist for the burn center and adult nutrition support at Vanderbilt University Medical Center, in Nashville, Tenn. “In that first week of critical illness, PN is not inferior to EN and does not cause more infections or worsen any clinical outcomes,” Dr. Cogle said. “So, should we start everyone on PN instead of EN? No, it is still more practical to use EN first if possible. But PN is an acceptable option if EN is not feasible.”
What about supplemental PN? The ASPEN guidelines do not recommend it in the first week of critical illness, stating that it has not been shown to improve clinical outcomes. The guidelines stress that clinical judgment should be used for malnourished patients and those with low lean muscle mass. But Dr. Cogle pointed out that of the six randomized controlled trials evaluated as part of the guideline process, none included malnourished patients.
“Indirect calorimetry was used to determine energy targets in one of those six studies, and predictive equations are only about 50% accurate in critically ill patients,” she said. “Supplemental PN is likely more beneficial in patients who are malnourished or are at high nutrition risk.”
Drs. Bliss and Cogle reported that they are advisors to Fresenius Kabi.
This article is from the February 2025 print issue.