Originally published by our sister publication Specialty Pharmacy Continuum
Most patients can continue taking glucagon-like peptide-1 (GLP-1) receptor agonists before undergoing elective surgery, according to new multi-specialty guidance from gastroenterologists, surgeons and anesthesiologists.
The recommendation (Surg Obes Relat Dis 2024;20[12]:1183-1186) is a reversal of previous, controversial guidance issued in 2023 by the American Society of Anesthesiologists (ASA) that advised a one-week break from injectable GLP-1 agents and a one-day break from once-daily oral agents. This initial recommendation was in response to several case reports of regurgitation and aspiration in patients on GLP-1s while under anesthesia, due to delayed gastric emptying attributed to the medication.
Collaboration, Risk Assessments Urged
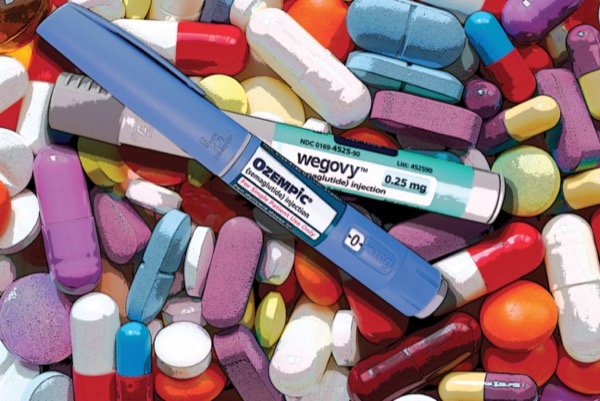
Stopping GLP-1 agents is not necessary for most patients, according to the new guidance. Instead, caregivers should assess patients’ risk for delayed gastric emptying and collaborate to decide if a short break is warranted. The authors added that withholding GLP-1 agents (Ozempic/Rybelsus/Wegovy, Novo Nordisk), liraglutide (Saxenda/Victoza, Novo Nordisk) and tirzepatide (Mounjaro/Zepbound, Eli Lilly) comes with its own set of risks, including hyperglycemia.
“These guidelines were issued in response to the fact that millions of people are now taking these drugs, and there have been reports of issues like gastroparesis-related aspiration that needed to be addressed,” said Ann M. Rogers, MD, the president of the American Society for Metabolic and Bariatric Surgery, one of the societies that coauthored the guidance. “Our goal is to heighten awareness of a potential safety issue to prevent it.”
“This concept of shared decision-making and developing local protocols is a foundational theme of this multi-society document, which builds upon our prior [recommendations] and other societal statements,” added Andrew Wang, MD, a gastroenterologist at the University of Virginia, in Charlottesville, one of the authors of the new guidance.
The new guidelines included recommendations for minimizing delayed gastric emptying, including preoperative diet modification and/or altering the anesthesia plan to consider rapid sequence induction of general anesthesia for tracheal intubation. To minimize aspiration risk, use a 24-hour liquid diet for patients undergoing colonoscopy and bariatric surgery. Additionally, a point-of-care gastric ultrasound could be used to assess aspiration risk, if available. If providers decide there is an unacceptable risk for delayed gastric emptying, they should follow the original guidance from the ASA, holding the day of surgery for daily agents and a week before surgery for weekly agents.
Dr. Rogers reported no relevant financial disclosures. Dr. Wang reported financial relationships with GE HealthCare Technologies and Pfizer.