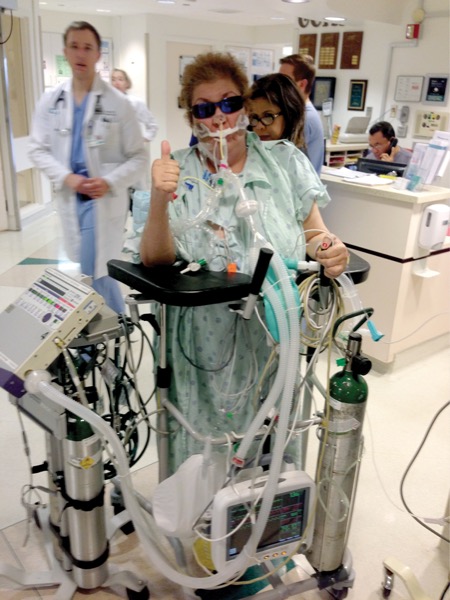
Early mobilization of patients in the ICU reduces episodes of delirium while strengthening their ability to complete activities of daily living after they leave the hospital, according to speakers at the Society of Critical Care Medicine (SCCM) 2025 Critical Care Congress, in Orlando, Fla. Some ICU patients experience prolonged sedation, which speakers stressed can be highly detrimental.
Early mobilization ranges from helping patients sit on the edge of their bed to assisted walking throughout the ICU floor, with nurses and physical therapists alongside for both mechanically ventilated and non-intubated patients. Mobilization is one element of SCCM’s ICU Liberation Campaign, also called the ABCDEF bundle. The bundle recommends ending sedation as soon as possible or at least lowering a patient’s amount of sedation promptly. Data collected via the SCCM’s ICU Liberation initiative show an association between implementing the bundle and a 68% decrease in seven-day hospital deaths, a 25% to 50% reduction in delirium and coma days, and a 50% reduction in ICU readmissions. A 46% reduction in hospital readmissions has also been reported (Crit Care Med 2019;47[1]:3-14).
But simply asking an ICU patient to get out of bed won’t cut it, reiterated Joanna Stollings, PharmD, a critical care pharmacist at Vanderbilt University Medical Center, in Nashville, Tenn. “Providers need to do the right kind of mobility, not passive range of motion or active range of motion,” she stressed. “We need to get patients sitting on the side of the bed, standing up, trying to walk across the room.”
Such efforts can be thwarted, however, by frequent shortages of physical therapists and occupational therapists, “which can make this hard,” Dr. Stollings noted. That said, she added that nurses and family members can help with early mobilization to get patients moving as soon as possible while saving the more complex patients for the physical or occupational therapists. And pharmacists have a role to play as well.
“Pharmacists are really big proponents of the ABCDEF bundle. It is my daily practice on rounds to assess if patients are a good candidate for early mobility and recommend to the team to consult physical and/or occupational therapy,” Dr. Stollings said. This includes people receiving vasopressors or extracorporeal membrane oxygenation, she said, adding that Vanderbilt has long championed early mobilization.
Culture Matters
Heidi Engel, DPT, a physical therapist for critical care patients at the University of California, San Francisco, warned against misinterpreting an ICU patient’s calm state as an indicator of health status. “A sedated patient looks really good; they’re very chill on the ventilator and they appear to be comfortably resting,” Dr. Engel said. However, the sedatives that seem to be bringing peace are actually causing harm, she noted, even if sedation only occurs for two days after ventilation.
“This is a medically induced comatose state,” which, among other harms, can cause delayed gastric emptying (Intensive Care Med 2008;34[3]:454-460) and potential intestinal obstruction, or induce delirium, Dr. Engel explained. That’s why it is so important to encourage patients to walk as soon as possible, within hours of starting ventilation if they can, she stressed. At the meeting, Dr. Engel showed a video of an ICU patient walking through the unit, ventilator intact, as music from San Francisco’s own Grateful Dead played in the background.
Changing Attitudes
Kali Dayton, DNP, AGACNP, a critical care nurse practitioner, has seen how important attitudes are to early mobilization adoption. In the beginning of her career, she worked in an ICU whose leaders valued the practice, and she soon saw the benefits for patients firsthand, including less delirium. Then she changed jobs to another ICU whose leaders were more likely to rely on sedation. It became an uphill battle to change the practice within the institution, so much so that Dr. Dayton decided to advocate for change another way. She transitioned to a consulting and training practice about the benefits of early ICU mobility, along with a podcast series (“Walking Home from the ICU”) and speaking engagements such as the Critical Care Congress.
Some ICU leaders embrace the value of early mobilization. “Together with partners in rehab and nursing, I have led our early mobilization program in the medical ICU at Yale New Haven Hospital for the past 10 years,” said Lauren Ferrante, MD, an associate professor of pulmonology and critical care medicine at Yale School of Medicine, in New Haven, Conn. Dr. Ferrante cited yet another study supporting the benefits of early mobilization in ICUs compared with not mobilizing patients (Respir Care 2016;61[7]:971-979).
The COVID-19 pandemic did prove to be a challenge, she noted, because caseloads that began to surge in March 2020 temporarily halted efforts at early mobilization of people in the ICU. By May of that year, however, “we were mobilizing ICU patients again, including patients with COVID-19,” Dr. Ferrante said, with personal protective equipment in place for clinicians to do this critical work safely.
The sources reported no relevant financial disclosures.
This article is from the May 2025 print issue.