Pharmacists all over the country are experiencing burnout in their jobs, which may negatively affect patient care and pharmacy students’ experiences on rotations. However, a team-based approach to topic discussions can reduce burnout while maintaining high-quality education for pharmacy students. When primary care pharmacists at Cleveland Clinic implemented this strategy, it proved to be a win for both learners and educators.
In the post-COVID era, concerns regarding burnout have been at the forefront, especially in healthcare. Burnout is an occupational phenomenon resulting from chronic workplace stress that has not been managed successfully. McQuade et al sought to understand the prevalence of burnout in health-system pharmacists during the COVID-19 pandemic and employed an electronic survey to better understand how pharmacists are affected.1 The second most reported cause of burnout was precepting requirements.
To decrease time burdens affecting preceptors, the Cleveland Clinic primary care pharmacists investigated an alternative model for delivering topic discussions. On advanced pharmacy practice experience (APPE) rotations, topic discussions occur during dedicated sessions for student learning that review disease states, pharmacology, clinical practice guidelines, and more. In the conventional method, a pharmacist conducts topic discussions in a one-on-one setting with a student. At our large academic health system, traditionally, 5 topic discussions per rotation are conducted for each student (diabetes - non-insulin, diabetes - insulin, hypertension, hyperlipidemia, and a specialty topic), resulting in a significant time commitment by individual pharmacists. Our goal was to draw on quality improvement program infrastructure with technology and a team-based approach to reduce the workload for pharmacists while maintaining a high level of instruction for APPE students.
In our system, ambulatory care pharmacists are embedded in primary care offices across a metro area. We determined the number of students who each pharmacist precepted in the 2023-2024 academic year. To predict the time spent conducting topic discussions using the traditional method, the total number of students precepted that year was multiplied by 5 hours to represent the standard topic discussions required per rotation. In the team-based approach, each pharmacist is responsible for leading 2 one-hour topic discussions per year via a virtual platform. Students completing APPE ambulatory care rotations are expected to attend and participate in virtual sessions.
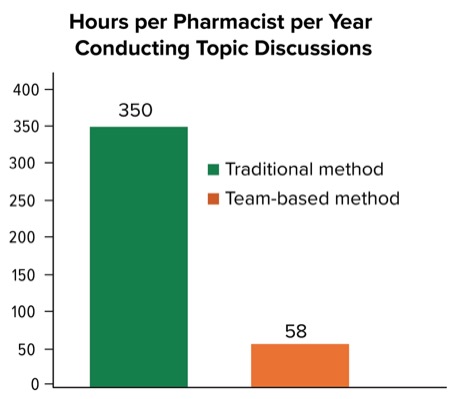
Over the course of the 2023-2024 academic year, 24 of 29 pharmacists precepted 70 students. We estimated that, under the traditional topic discussion method, assuming each topic discussion is 1 hour in length, 350 pharmacist hours per year would have been spent conducting topic discussions. However, using the team-based approach, each pharmacist spends 2 hours per year conducting topic discussions, totaling 58 pharmacist hours per year. We concluded that this group of 29 pharmacists is saving 292 hours per year by using a team-based approach to topic discussions (Figure).
The purpose of the project was to investigate an alternative model for delivery of topic discussions to decrease time burdens affecting pharmacists. It is evident that the team-based approach saves the pharmacists time. The time saved may fluctuate based on pharmacist team size and the number of students completing APPE rotations at any given institution.
Our team found a benefit to the topic discussion schedules set well in advance, which prevented scrambling to work the topics into an individual pharmacist’s schedule for every rotation. Students also have the opportunity to learn from pharmacists beyond their own preceptor. Group topic discussions provide students with the opportunity to collaborate with those from other universities and learn from each other while also providing insight to preceptors regarding how students interact with their peers. The team-based approach also provides a more structured and standardized instructional method ensuring that all APPE students are provided a similar experience at Cleveland Clinic.
One disadvantage of the team-based approach is the need for using a virtual platform, which may not be the best strategy for some students. Also, it may be difficult to identify struggling students because stronger ones dominate during participation portions of the sessions.
Overall, we have seen many benefits to the team-based approach for both our pharmacists and students. The new structure is intended to save pharmacists’ time, which may decrease burnout. Healthcare institutions should continue to look for methods where technology can be used to decrease time burdens while still providing a high level of education and training for learners.
Dr. Parker is a primary care pharmacist at Cleveland Clinic. Lauren Schultz, PharmD, BCACP, and Olivia Ojeda, BS, were also instrumental to leading the project.
Reference
- McQuade BM, Keller E, Elmes A, et al. Stratification of burnout in health-system pharmacists during the COVID-19 pandemic: a focus on the ambulatory care pharmacist. J Am Coll Clin Pharm. 2022;5(9):942-949.nonbreaking space