Originally published by our sister publication Specialty Pharmacy Continuum
By Gina Shaw
Healthcare is increasingly being provided in the home, and that means more medical devices are also being used in the home—making usability challenges for home operators the No. 1 health technology hazard of 2024, as identified by the Institute for Safe Medication Practices (ISMP) and ECRI.
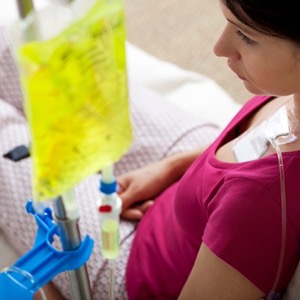
“These devices are often not designed for home users, and they may lack the expertise to operate the device properly,” said Rob Schluth, the principal project officer for product development in ECRI’s Device Evaluation Group. “The home environment can also be a factor, with space restrictions, cleaning and disinfection limitations, and power supply reliability and electrical safety.”
As a result, undetected medical events and errors can occur; results can be misleading or misinterpreted; or there may be an inappropriate response to a malfunction, all of which can lead to patient harm. “For example, consider infusion pumps,” Mr. Schluth said. “Misprogramming of the pump can lead to medication errors or delayed care, or if the cap is not removed from the infusion line, improper medication delivery can result.”
To prevent errors like these, ECRI recommends that providers:
• select devices that are well matched to the patient and their home environment;
• train users on proper device operation and provide instructional materials; and
• assign a liaison specifically tasked with addressing questions that patients may have about using their device.
Among the other top 10 health technology hazards that particularly involve pharmacy practice are:
No. 3: Sterile drug compounding without the use of technological safeguards increases the risk for medication errors.
“If not caught in the pharmacy, compounding errors have a high likelihood of reaching the patient and can be fatal,” Mr. Schluth said, noting that pharmacies should implement technological safeguards that minimize the risk for human error. He advised pharmacists to look for systems that offer:
- barcode verification of all source products;
- tools for guiding users through essential steps;
- remote verification of steps via images, video and/or gravimetric analysis;
- the ability to interface with the electronic health record; and
- automated calculations and conversions.
“As medication safety experts who provide and support care on the front line, pharmacists should champion safe practices for barcode administration and support an escalation process when a barcode does not scan,” Mr. Schluth said.
No. 8: Infusion pump damage remains a medication safety concern.
“Infusion pumps can become damaged over time from frequent handling or mishandling, exposure to cleaning chemicals, and just normal wear and tear,” Mr. Schluth said. “Pumps should not be used if there is any visible damage, any part of the setup seems abnormal or if an unresolvable alarm condition occurs.”
He urged pharmacists to help build a better system for health technology safety. “Find out how technology problems are reported within your organization and share that information with your colleagues,” he said.“Become an advocate for safe technology stewardship: communicating adverse events, near misses and other concerns; investigating causes; and sharing solutions.”