By Donavyn Coffey
Approximately 10% of all U.S. patients carry a penicillin allergy label. The majority pick up the label in childhood after an adverse reaction or because a family member is labeled allergic. But the reality is that fewer than 1% of these patients have true IgE-mediated sensitivity to the antibiotic, according to data cited by the Centers for Disease Control and Prevention. And even the true penicillin allergies are often outgrown (JAMA 2017; 318[1]:82–83).
This leaves a significant population of children and adults barred from first-line treatments unnecessarily, according to Christine MacBrayne, PharmD, an antimicrobial stewardship and infectious disease clinical pharmacist specialist based out of Colorado. These patients rely on suboptimal antibiotics with side effects and higher costs (JAC Antimicrob Resist 2022;4[6]:dlac116).
Delabeling is a low-risk way to get them better care, Dr. MacBrayne noted at the 2023 ACCP Annual Meeting, in Dallas. Given the higher costs and worse outcomes that come with a penicillin allergy label, delabeling is important for patient safety.
“Many people carry around penicillin allergies out of fear of anaphylaxis,” Dr. MacBrayne said. Therefore, parents will label their children as allergic because their siblings or parents are. Caregivers may even inflate negative reactions to penicillin in an effort to protect their child, she said.
But it’s important, as pharmacists, to explain to these caregivers that a negative drug reaction such as a rash does not confer an allergy. In fact, the most common negative reactions, such as diarrhea, “can often be a result of the nonselective killing of targeted bacteria,” she said.
Moreover, anaphylaxis, while severe and potentially life-threatening, will usually happen within one hour of encountering the allergen (J Adv Pharm Technol Res v.1[1];Jan-Mar 2010).
3 Steps to Delabeling in Ambulatory Care
Some allergy labels can be removed based on clinical history alone. Data in both adults and pediatric patients has shown that after screening with a targeted questionnaire, many patients have no clear reason for a penicillin allergy label.
If a patient avoids penicillin based on family history or has tolerated penicillin or a related drug since the incident, a patient is considered at no increased risk and can be delabeled. “No skin test or drug challenge needed,” Dr. MacBrayne said.
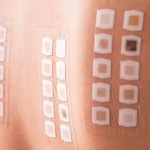
If they can’t be ruled out by history alone, pharmacists can move on to skin testing as recommended by the International Consensus on Drug Allergy. If the skin test is negative, proceed with an oral challenge with a 60-minute observation, she said.
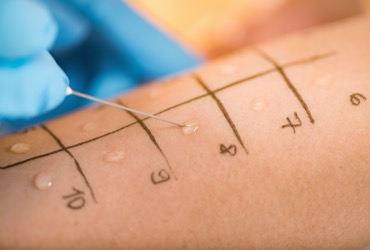
Because skin testing can result in a multistep process within ambulatory care, it may be appropriate to move straight to oral challenge in low-risk patients.The low-risk category includes anyone whose reaction occurred more than 24 hours after exposure to a penicillin-based antibiotic and had symptoms that were not progressive, such as gastrointestinal issues or a rash alone, Dr. MacBrayne said.
In a 2023 prospective study of penicillin delabeling by graded oral challenge in the pediatric primary care setting, 21 in 23 patients exhibited no delayed or immediate reaction to the oral challenge (Ann Allergy Asthma Immunol 2023;130[5]:P667-669). A meta-analysis concluded that delabeling can be done in a significant number of patients without skin testing. The authors also determined that penicillin allergy delabeling by a non-allergist is not only safe but efficacious (Int J Infect Dis 2023;129:152-161).
“Removing the allergy in patients who are at no increase or low risk is the safest choice,” Dr. MacBrayne said.
Dr. MacBrayne reported no relevant financial disclosures.